New Street Medicine Program addresses urgent need in Scranton

Dr. Tejas Nikumbh, far left, a resident physician in The Wright Center for Graduate Medical Education’s Internal Medicine Residency Program, and far right, Dr. Douglas Klamp, The Wright Center’s senior vice president, chief medical education officer, and physician chair of resident and fellow talent acquisition, treat patient Tyler Worden as part of a new street medicine program launched by The Wright Center.
The Wright Center for Graduate Medical Education’s new initiative provides resident physicians with experience treating underserved populations
As he walked toward the mobile medical clinic parked at a homeless shelter in Scranton on a frigid morning in early January, Dr. Tejas Nikumbh wasn’t sure what to expect.
Within minutes, patients began lining up outside The Wright Center for Community Health’s 34-foot mobile medical and dental unit known as Driving Better Health, hoping to see a doctor. There had been no advertising and no announcements about the new street medicine team – just word of mouth and a deep need for medical care.
“We just showed up, and they were waiting for us. We saw about 15 patients within that first two and a half hours,” said Dr. Nikumbh, a resident physician in The Wright Center for Graduate Medical Education’s Internal Medicine Residency Program. “It was so satisfying, because we had worked so hard to get to that first visit.”
For more than 18 months, Dr. Nikumbh and his colleagues have worked to launch a program to help people experiencing homelessness. As The Wright Center’s leaders worked to secure funding and infrastructure, he and other resident physicians joined medical students from the region to provide basic medical services at the Community Intervention Center (CIC) on North Sixth Avenue, a daytime shelter near downtown Scranton that provides a variety of services to people experiencing homelessness.
Four months later, The Wright Center’s Street Medicine Team, led by Dr. Douglas Klamp, senior vice president, chief medical education officer, and physician chair of resident and fellow talent acquisition, have completed more than 365 medical exams aboard Driving Better Health. The team, composed of medical assistants, community health workers, addiction recovery specialists, resident physicians, and more, visits the CIC twice a week to offer medical appointments on a first-come, first-served basis.
A five-year, $500,000 grant from the U.S. Health Resources and Services Administration’s (HRSA) Bureau of Health Workforce supports the program, which aims to educate Internal Medicine resident physicians and faculty about caring for people experiencing homelessness. With funding secured in 2025, The Wright Center began assembling a team and planning how to combine education with action.
More than 220 people in Lackawanna County are experiencing homelessness, according to the 2025 U.S. Department of Housing and Urban Development Point in Time report. The CIC reports nearly 500 unsheltered people on its roster.

Tejas Nikumbh, left, a resident physician in The Wright Center for Graduate Medical Education’s Internal Medicine Residency Program, and Dr. Douglas Klamp, center, The Wright Center’s senior vice president, chief medical education officer, and physician chair of resident and fellow talent acquisition, talk with patient Erylene Cooke aboard the 34-foot mobile medical and dental unit known as Driving Better Health.
“Many of the individuals we serve face significant barriers to accessing healthcare, including transportation issues, lack of insurance, mental health challenges, homelessness, and distrust of traditional systems,” said Michelle Matyjevich, deputy director of the CIC. “Bringing services directly to them in a familiar and welcoming environment has helped remove many of those barriers.”
The services the street medicine team offers, including the educational experience provided to resident physicians, are at the heart of The Wright Center’s mission.
“With anything in the field of medicine, learning about something in a lecture hall does not teach you the important little details,” Dr. Klamp said. “We have the means to go out and meet people where they are, which gives our medical residents a deeper understanding of all the obstacles people experiencing homelessness face.”
‘They’re unseen’
Treating people without access to healthcare is deeply personal for Dr. Nikumbh. Growing up in Mumbai, India, he watched his father, a dentist, regularly care for patients who could not pay for services. His mother, who worked in a bank, told him that being “a good man” was of great importance, no matter what career he chose.
After graduating from medical school, he worked as a surgeon in India before moving to the United States. In 2023, Dr. Nikumbh began his three-year Internal Medicine Residency at The Wright Center. In addition to wanting to train in an academically rigorous program, he was interested in providing whole-person primary and preventive health services in medically underserved communities.
As he began clinical rotations at The Wright Center’s community health centers and regional hospitals, Dr. Nikumbh joined a small group of like-minded medical residents in asking The Wright Center’s leadership team how they could create a program to deliver care to people without reliable access to health services. Together, they developed a community-oriented primary care initiative focused on understanding the needs of people experiencing homelessness in Lackawanna County. They also enlisted the support of Dr. Klamp, whose experience caring for vulnerable populations overseas dates back to the 1980s.
Meanwhile, Dr. Nikumbh and other resident physicians continued to make regular visits to the CIC to provide basic medical services, including blood pressure checks and glucose testing. This helped build a foundation for the street medicine team’s first visits with Driving Better Health.
“The No. 1 thing I’ve realized is that the people who need these services are neglected. They’re unseen,” Dr. Nikumbh said. “So, when they meet someone who cares, they will open up. I’ve given many of these patients my cell phone number, so they know who they can call when they need help.”
Building those kinds of relationships is the key to impacting their health, according to Matyjevich.
“Meeting people where they are – physically and emotionally – has made a tremendous difference,” Matyjevich said. “The mobile medical unit and outreach approach create a more comfortable, approachable environment where people are more willing to engage. The team’s consistency, compassion, and willingness to build relationships over time help establish trust, which is critical when working with vulnerable populations.”
‘Meet their basic needs’
As a Federally Qualified Health Center Look-Alike, The Wright Center’s services go beyond delivering whole-person primary and preventive health services. For instance, community health workers help patients and community members with enrolling in health insurance, transportation to doctors’ appointments, utility bills, accessing food and clothing, and connecting patients with community resources. These specialized employees, along with addiction support specialists, behavioral health workers, and more, join the street medicine team for each visit to the CIC.

Ivy Nataloni, left, a community health worker at The Wright Center for Community Health, meets with patient Erylene Cooke as part of The Wright Center’s new street medicine program.
The team helped one patient with chronic back pain obtain a hammock so he could sleep more comfortably outside, Dr. Nikumbh said. Others received bus passes to get to and from appointments, gift cards for groceries, and connections to other vital community resources.
“Hunger takes precedence, that’s been the biggest lesson for me,” he said. “We have to be innovative in the way we support these patients, to work together to find ways to meet their basic needs so they can focus on improving their health.”
The experience is also reshaping how The Wright Center’s resident physicians and staff understand homelessness. Dr. Klamp said one of the first lessons for new team members is that many common assumptions about people experiencing homelessness are rooted in myth.
“A very high number of the patients we’re treating have held jobs for most of their lives and had homes and families,” he said. “For many, homelessness is not a permanent situation. They just need some support.”
Residents who work on the mobile medical and dental unit are also getting real-world education about the cost of prescription medicines and how difficult it is to access them, Dr. Klamp said. The residents encounter many patients who are not taking medications for chronic illnesses, including diabetes, heart disease, high blood pressure, and chronic obstructive pulmonary disease. Not taking medication regularly can turn small health issues into larger problems, he added.
‘For the greater good’
In the few months since the street medicine team began visiting the CIC, staff there have noticed the impact.
“We have seen increased engagement from individuals who otherwise would not seek medical attention on their own,” Matyjevich said. “People are receiving basic medical care, blood pressure and blood sugar checks, medication support, referrals, and follow-up care that may have otherwise gone untreated.
“Just as importantly, the presence of The Wright Center team has helped build trust and consistency with a population that often struggles to maintain ongoing healthcare relationships.”
In addition to making bi-weekly visits to the CIC, The Wright Center’s resident physicians are participating in regular educational sessions to learn more about treating vulnerable populations they may not encounter regularly in the clinics and hospitals where they complete clinical rotations. As the educational curriculum around street medicine evolves, leaders want to feature weekly sessions featuring real-life stories from patients treated on Driving Better Health, so resident physicians can analyze cases and find ways to improve care.
Just days into the project, the response to the street medicine team’s visits to the CIC had already surpassed expectations, according to Dr. Klamp, making one thing clear: The services must grow. In addition to expanding the team’s schedule, Dr. Klamp and the team hope to bring Driving Better Health to more locations, extending its reach to even more individuals in need.
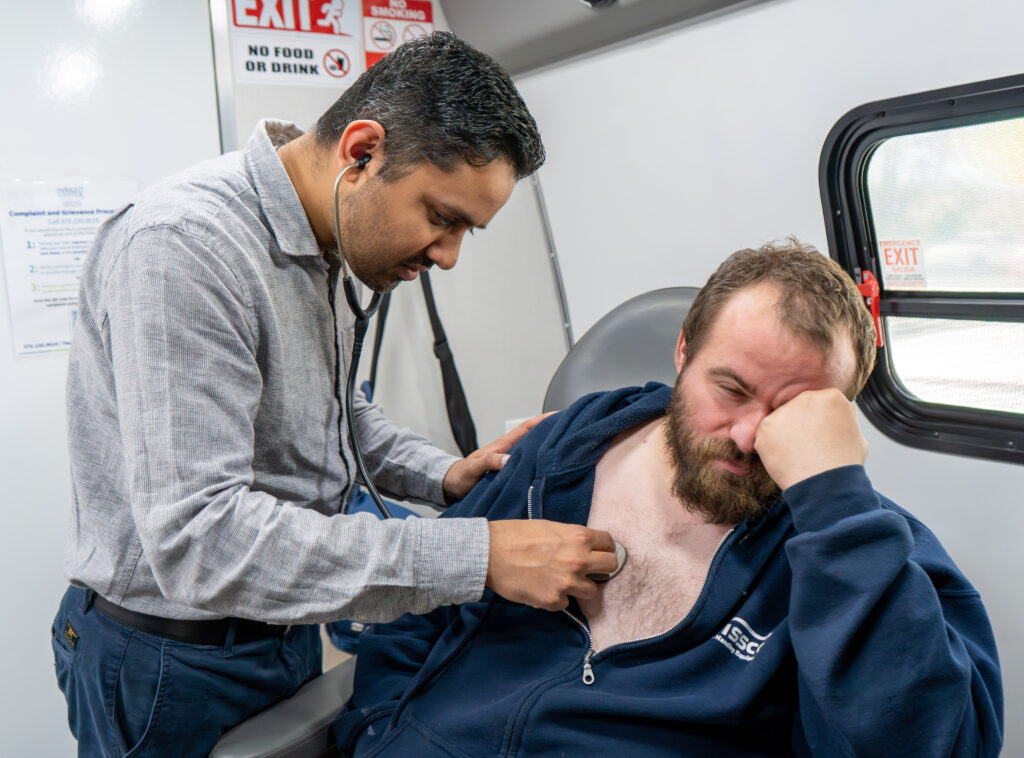
Dr. Tejas Nikumbh, a resident physician in The Wright Center for Graduate Medical Education’s Internal Medicine Residency Program, examines patient Tyler Worden during a stop at Scranton’s Community Intervention Center. Since January, staff and resident physicians at The Wright Center have visited Scranton’s Community Intervention Center twice a week, completing more than 365 medical exams aboard the 34-foot mobile medical and dental unit known as Driving Better Health.
In June, Dr. Nikumbh will graduate from the Internal Medicine Residency Program. He plans to work as an academic hospitalist at St. Francis Hospital in Hartford, Connecticut, to be closer to his wife, Sanika, who is completing a radiology residency, and their infant daughter, Avanti. He will also serve as an assistant professor in internal medicine at the University of Connecticut. He plans to continue working with people in need during his spare time, and hopes the team he helped start here will continue to grow.
“We hit a lot of barriers in our journey to launch this program, but having the conviction that we are doing something for the greater good helped us keep going,” Dr. Nikumbh said. “It’s important to make this program sustainable so we can continue to do good in our communities.”

































