Our Mission, Vision and Values Make the WRIGHT Difference
Learn about our organization and the people who make it great.
Learn MoreLearn about our organization and the people who make it great.
Learn MoreFor more than 45 years, we’ve been committed to providing safety-net care to vulnerable populations while training the next generation of primary care physicians.
Our History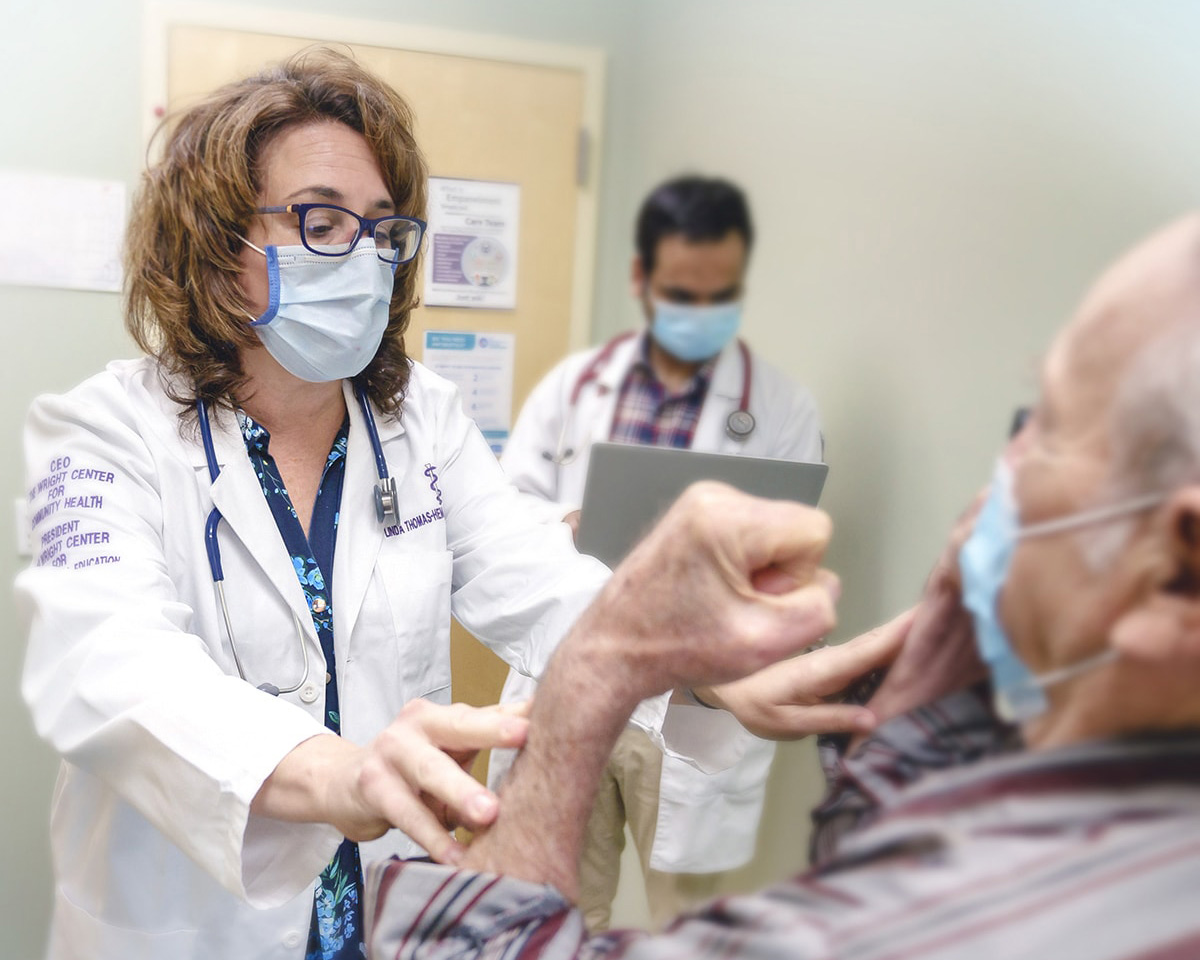
What does a Federally Qualified Health Center mean for you?
Learn MoreOur shared purpose isn't only local, it’s state and nationwide.
Learn MoreEvery member of our leadership team shares a passion for providing the highest quality health care to our community.
Learn MoreOur organization is led by engaged and diverse board members, including patients, staff members, and community advocates.
Learn MoreOur commitment to the region transcends the walls of our clinical locations and learning environments by spurring economic growth and development in our surrounding environs.
Learn MoreThe Wright Center for Patient & Community Engagement exists to educate and advocate for patients to create the best experience possible.
Learn More