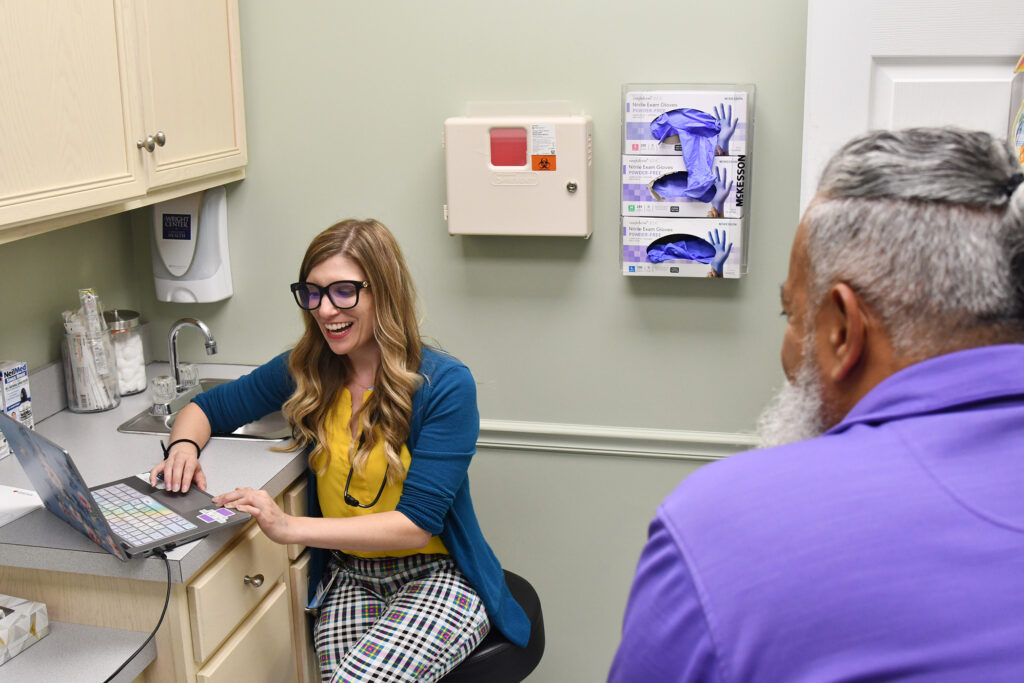
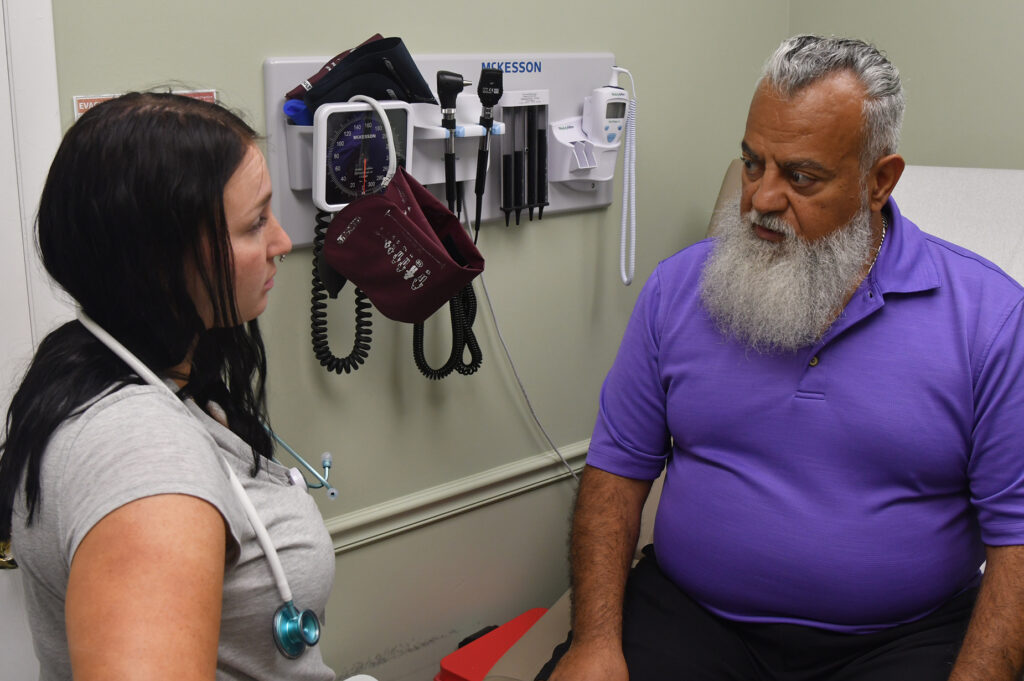
A dentist who completed his residency with The Wright Center for Community Health will see patients at the newly expanded dental wing at the nonprofit’s community health center in Wilkes-Barre.

Michael Regan, D.M.D.
Dr. Michael Regan began seeing patients on Tuesday, Aug. 6, at 169 N. Pennsylvania Ave. The expanded dental clinic – the largest in The Wright Center’s regional network – is part of recently completed renovations that added 7,700 square feet of space to The Wright Center for Community Health in Wilkes-Barre.
The new dental wing features cutting-edge technology, including an Orthopantomograph 3D LX that provides 3-D dental imaging. The machine can take a single panoramic X-ray of the teeth, mandible, and maxilla, giving clinicians more detail as they diagnose and treat patients.
Dr. Regan completed his postdoctoral Advanced Education in General Dentistry residency at The Wright Center’s community health center in Scranton through an affiliation with New York University Langone Health’s Dental Medicine Postdoctoral Residency Program. The well-known program is the world’s largest postdoctoral dental residency program of its kind, training about 400 dental residents annually at partner sites in nearly 30 states.
After working closely with The Wright Center’s dental staff and seeing firsthand the growing need for dentists in Northeast Pennsylvania, Dr. Regan knew he wanted to stay here and help fulfill The Wright Center’s mission to improve the health and welfare of our communities through health services and the sustainable renewal of an inspired, competent workforce that is privileged to serve.
Dental hygienists Jenna Topa and Samantha Solack will support Dr. Regan.
The Wright Center accepts all dental insurance. To ensure high-quality oral care is available to everyone, The Wright Center for Community Health offers a sliding-fee discount program to individuals who qualify based on Federal Poverty Guidelines that take into account family size and income. No patient is turned away due to an inability to pay.
The community health center is open Monday through Saturday from 8 a.m. to 6 p.m. To make an appointment, call 570-491-0126 or visit TheWrightCenter.org.
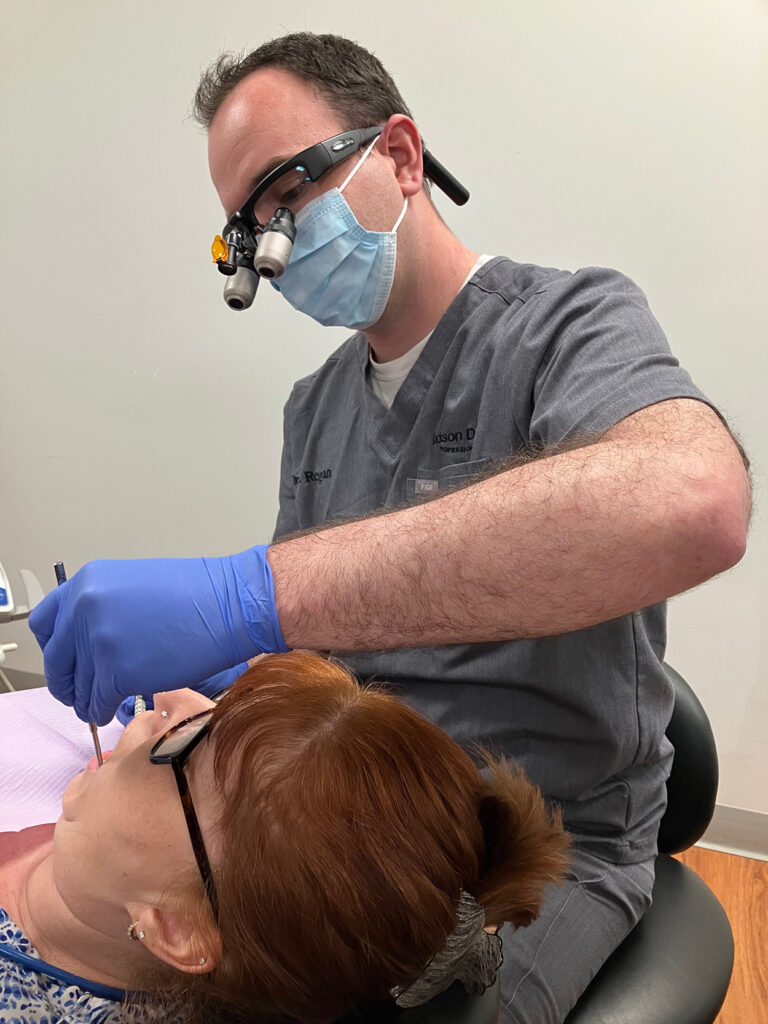
Dr. Michael Regan is seeing dental patients at The Wright Center for Community in Wilkes-Barre, 169 N. Pennsylvania Ave. The recent expansion in Wilkes-Barre enables the community health center to see patients Monday through Saturday from 8 a.m. to 6 p.m.
The community health center in Wilkes-Barre opened its doors to patients on Jan. 9, 2023. Since then, a multiphase expansion project has proceeded inside the 34,460-square-foot facility, a former office building only blocks from the city’s downtown business district.
The Wright Center, headquartered in Scranton, has a growing network of 12 community health centers in Lackawanna, Luzerne, Wayne, and Wyoming counties, including a mobile medical and dental unit called Driving Better Health. Its locations offer affordable, high-quality, nondiscriminatory, whole-person primary health services to people of all ages regardless of their insurance status, ZIP code, or ability to pay. Patients typically have the convenience of going to a single location to access integrated medical, dental, and behavioral health care, as well as community-based substance use disorder treatment and recovery services.